What to expect
Here’s What To Expect
The initial consultation and treatment will last approximately 1 hour. This will involve a detailed case history, which will include any previous medical history such as any serious illnesses, accidents, broken bones, or operations which you have had since birth up to the present day. Any of these may have a bearing on your current problem.
An examination will then be carried out and you may be asked to perform simple movements to aid in the understanding and assessment of your situation. In addition other tests such as blood pressure, reflexes, joint mobility and muscle strength may also be performed.
A diagnosis will be made based on your case history and examination findings; this will then be discussed with you before beginning treatment. The Osteopath may ask you to visit your doctor or suggest other treatments or investigations which may be helpful in solving your problem.
A treatment plan will be made if osteopathic treatment is indicated which will also incorporate advice on diet, lifestyle and exercise.
Sometimes more than one session is needed in order to not only relieve pain but to rehabilitate and help prevent future recurrences of the problem. Additional treatment sessions are half an hour. At any time during your appointment you can ask your osteopath to stop treatment and explain anything they have said or any techniques performed. As with your GP, all personal and clinical information is dealt with in the strictest confidence.
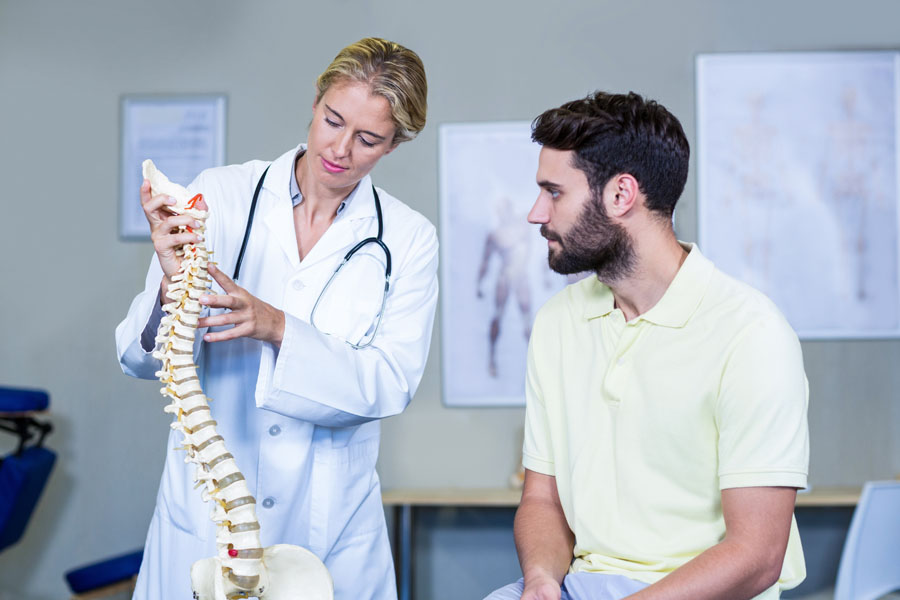
What to expect from your first visit.
- You will be seen by a fully qualified and registered osteopath. If you have a preference as to who you see whether this is
- The first session will last approximately 60 minutes, and further sessions will last approximately 30 minutes (these sessions are longer during the pandemic to give time for the room to be aired and cleaned)
- Your Osteopath needs to know about your health, past and present. As part of this you will be asked detailed questions about your current complaint, medical history, general health and any medication you are taking.
- The osteopath will discuss your situation with you and together you will decide the best way to proceed and what examinations would be useful to help evaluate what is going on.
- You will be asked to consent to all examinations and treatment. The reasons for them will be clearly explained and alternatives offered. Nothing will be done that you are not aware off or happy with.
- A physical examination is carried out, sometimes incorporating medical equipment to help with your assessment and diagnosis.
- You maybe ask to remove some of your clothing to perform a simple series of movements. There is a screen to change behind or the Osteopath may leave the room as you undress. Keep on as many clothes as you feel comfortable with. Tight restrictive clothes can make examination and treatment difficult and may affect the effect the effectiveness of your treatment. We advise loose clothing and have shorts, t-shirts and gowns available to wear if you would prefer. Your need to be comfortable at all times.
- You may bring a chaperone with you, this can be a friend or relative.
- The findings from the case history and examination will be discussed with you and a treatment plan that you happy with and understand given.
- Osteopaths use touch to identify key points of weakness or excessive strain in the body. You will usually be treated lying down on a treatment couch.
- Osteopaths usually start any treatment by releasing and relaxing muscles and stretching stiff joints using gentle massage techniques, rhythmic joint movements and muscles release techniques. They may also carry out spinal manipulations. These are short quick movements to joint in order to help them restore normal joint function and mobility. A lot of the Osteopaths in the clinic also use acupuncture. All treatment options will be discussed and alternatives offered and consent asked for.
- You and your osteopath may decide that a home program would be appropriate to reinforce any work in the session or to speed up your recovery. This can be advice or exercise.
- Sometimes it is possible to feel a little sore after a treatment session depending what techniques are done. This should not be painful but a little ache is common. It normally does not last more than 24-48 hours. Anything more than this please let us know straight away. Most reactions are proportional amount of treatment (and techniques used) your receive. Tall efforts will be made to minimise this. All treatment options will be discussed and decided on together by your and the osteopath before treatment.
- A prognosis is given with expected time scales. This will be revisited and modified on subsequent visits as the osteopath can see how you have reacted to treatment.
- If after the assessment or after a few treatment sessions, you or the osteopath feel a different specialist maybe more appropriate then an onward referral will be made. You can withdraw consent or stop treatment at any time. We will do all we can to help your as quickly and efficiently as we can.
- We hope you enjoy your session and welcome all feedback.
